Summary:
- The largest Ebola Virus Disease (EVD) outbreak in West Africa caused 11,325 deaths.
- It is transmitted from wild animals and spreads through human-to-human mainly by blood and body fluids, caused fatal dehydration and organ failure.
- Inappropriate selection and improper use of PPE are among reasons which caused deaths of medical personnel.
- ULTITEC 2000 and ULTITEC 3000T qualified based on guidance on PPE in CDC Infection Control Program.
Democratic Republic of Congo (DRC) declared tenth outbreak of Ebola in 40 years on August 2018, which caused 1,630 deaths as of July 2019. While across the border, Ugandan authorities are bracing for possible outbreak of the deadly virus as few travelers died after returning from DRC. Ebola Virus Disease (EVD), formerly known as Ebola Hemorrhagic Fever, was first discovered in 1976. The virus is transmitted from wild animals (fruit bats, chimpanzees, monkeys etc.) and spreads through human-to-human transmission. The largest Ebola epidemic ever recorded was the West Africa Outbreak in 2014, which ended with 28,652 suspected cases and 11,325 deaths in 2016.
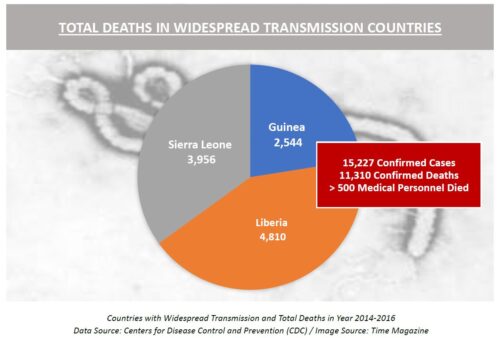
From Ebola Disease to Pandemic Threat
According to Centers for Disease Control and Prevention (CDC), of the 15,227 confirmed cases in Guinea, Liberia and Sierra Leone, more than 500 medical personnel died due to EVD. Liberia lost 8% of its doctors, nurses, and midwives to EVD. The outbreak has also claimed the lives of doctors, nurses, and technicians from Mali, Nigeria, Spain, and the United States. It impacted the provision of healthcare services and caused treatment and control setbacks of malaria, tuberculosis, HIV, and measles in these countries too

Symptoms and Transmission Mode of Ebola
The EVD incubation period is from 2 to 21 days. An infected Ebola patient cannot spread the disease until they develop symptoms namely fever, fatigue, muscle pain, sore throat followed by vomiting, diarrhea, rash, internal and external bleeding etc. Fatal dehydration and multiple organ dysfunction will occur in acutely ill patients which then lead to deaths.
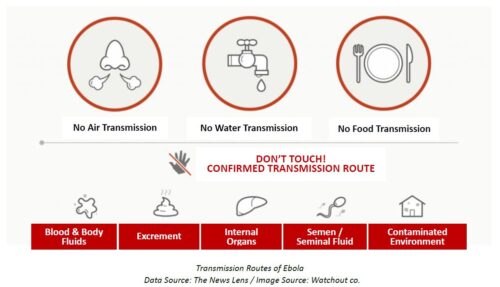
Guidance on Personal Protective Equipment (PPE) for Infection Control
The EVD is a serious occupational health and safety risk for medical personnel. Several factors explain the high proportion of infected medical personnel, includes shortages of PPE, improper selection and usage of PPE, insufficient medical personnel, long working hours etc. The case fatality rate of Ebola is 50 to 90% which is far higher than 2009 influenza pandemic (0.01%) and SARS (9.6%).
According to CDC, PPE that fully covers skin and clothing is recommended to prevent exposure of eyes, nose, and mouth. This reduces the risk of accidental self-contamination of mucous membranes or broken skin. All PPE used must adhered to infection control program that follows CDC recommendations and Occupational Safety and Health Act of 1970 (OSHA) requirements. Medical personnel should heighten vigilance, wear standard protective equipment and practice strict infection control, including hand and respiratory hygiene. When entering a ward where a suspected or confirmed case is isolated, advanced PPE such as coveralls, masks, face shields, apron, double gloves, water-proof boot covers are required.
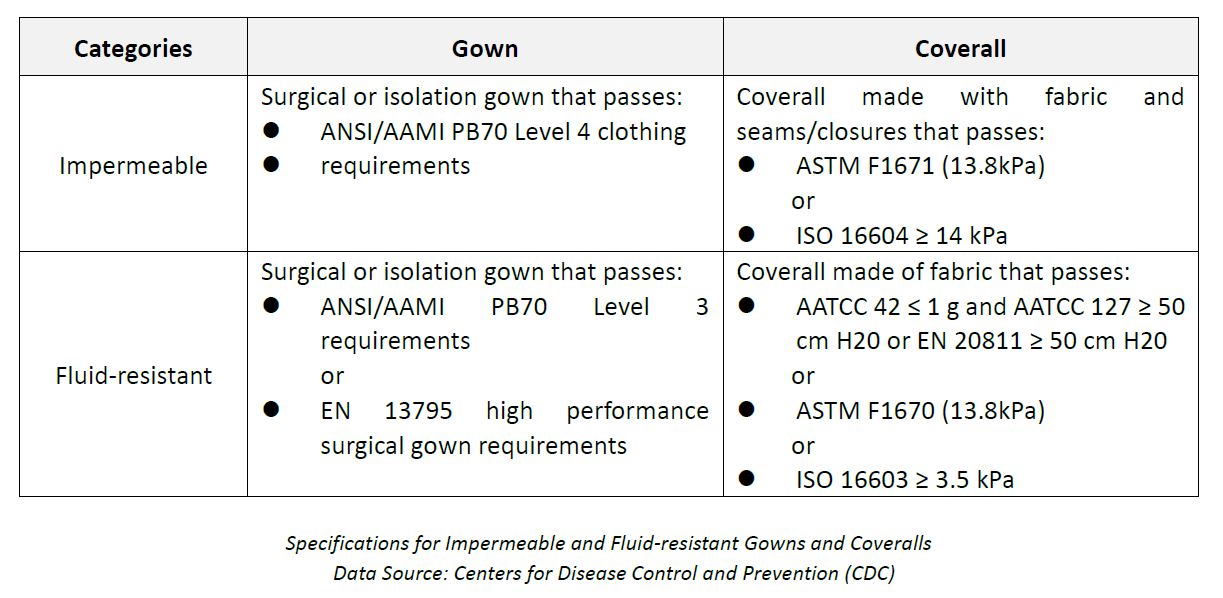
Specifications for Impermeable and Fluid-resistant Gowns and Coveralls
There are sections outline requirements for gown and coverall, but selection of PPE is only part of the EVD infection control program. Impermeable gown and coverall indicate the material and construction have demonstrated resistance to synthetic blood and simulated bloodborne pathogens. Fluid-resistant indicates a gown that has water resistance or a coverall that has water or synthetic blood resistance.
There are two fluid-resistant coveralls fully meets above requirements of ASTM F1670 and ISO 16603, namely ULTITEC 2000, ULTITEC 3000T and ULTITEC 4000 , which are appropriate for disease control and disaster management. Their premium microporous fabric offers outstanding barrier against blood, body fluids and infective agents while maintaining breathability and comfortability. According to CDC, trained observers are required to ensure PPE is being used appropriately in donning, patient room and doffing area. The donning and doffing protocols are strictly adhered to a checklist to eliminate contamination of own clothing and ensure safe return of medical personnel.
In conclusion, EVD is an important occupational safety lesson for worldwide which caused serious health, social and economic consequences to affected countries. Although the spread of EVD in West Africa has been controlled, and experimental vaccines have been used to control outbreaks in DRC and Uganda, additional cases may continue to occur at anytime and from anywhere. However, due to ongoing surveillance and strengthened response capabilities, each country should have the experience and tools on Ebola outbreak preparedness to identify cases and limit the spread of the disease in future.
Reference:
- WHO: https://www.who.int/en/news-room/fact-sheets/detail/ebola-virus-disease
- CDC: https://www.cdc.gov/vhf/ebola/healthcare-us/ppe/guidance.html
- Barcelona Institute for Global Health (ISGlobal): https://www.isglobal.org/en/ebola
- The News Lens: https://www.thenewslens.com/article/10011

